$1 trillion in cuts put rural hospitals at risk
Writer: Mirella Franzese
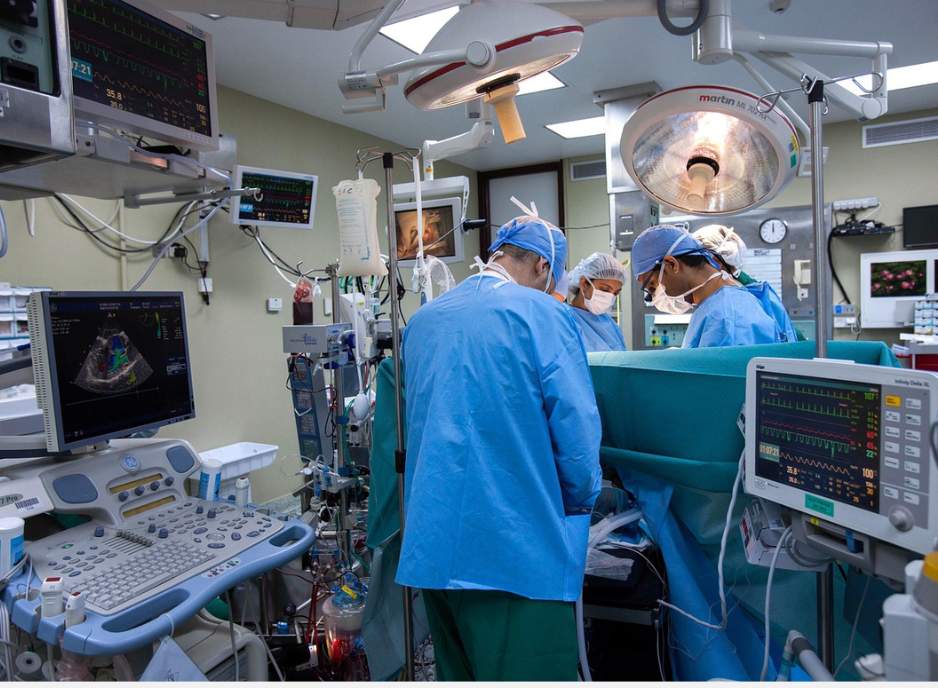
August 2025 — President Trump’s recently passed key legislation, referred to as the “Big Beautiful Bill,” is expected to cut $1 trillion in federal health spending over the next decade, triggering what health policy analysts warn could be a crisis for rural hospitals and low-income Americans.
Underserved regions are projected to absorb $155 billion of the total cuts over a 10-year period, according to independent health researcher KFF.
Rural hospitals, many of which rely on Medicaid and Medicare reimbursements for maintaining operations, could see a $70 billion reduction in funding under the legislation.
American Hospital Association CEO Rick Pollack called the reductions the largest ever put forward by Congress.
“The real-life consequences of these nearly $1 trillion in Medicaid cuts…will result in irreparable harm to our health care system, reducing access to care for all Americans and severely undermining the ability of hospitals and health systems to care for our most vulnerable patients,” said Pollack in a press release.
KFF projects as many as 17 million Americans could become uninsured by 2034 due to new federal work requirements for Medicaid eligibility and the expiration of the Affordable Care Act’s enhanced premium tax credits.
Additional ACA changes include a shorter annual open enrollment period, the replacement of automatic enrollment with manual re-enrollment, and the elimination of the low-income special enrollment period. More than 3 million beneficiaries could lose coverage from these new technical requirements.
In rural areas, where Medicaid enrollment is high and access is challenging due to long travel distances and staff shortages, these new measures threaten the ability of local hospitals to provide quality and accessible health solutions for residents.
Nearly one-third of rural hospitals nationwide are at risk of closing due to financial constraints, according to a report by Time. The cuts would reduce state support for treating Medicaid patients and increase the financial burden of caring for uninsured patients, pressuring more rural hospitals toward closure.
“(The cut) will force hospitals to make service line reductions and staff reductions, resulting in longer waiting times in emergency departments and for other essential services,” explained Pollack. “(That) could ultimately lead to facility closures, especially in rural and underserved areas.”
The Oklahoma Hospital Association, for instance, recently announced the closure of a member hospital. These closures are “coming because part of this is that hospitals have relied on these special Medicaid payments in order to be able to have a bottom line at the end of the year,” Rich Rasmussen, president and CEO of the Oklahoma Hospital Association, told U.S. News.
While the bill allocates $50 billion to help rural hospitals grapple with financial losses from Medicaid cuts, health systems are likely to still fall short of covering expected losses. Half the funding would be split evenly between approved states, while the remaining $25 billion would be allocated to the 1,800 rural hospitals based on factors such as the share of rural residents, the number of rural health facilities, the presence of disproportionate-share hospitals, and other criteria set by the program administrator.
KFF estimates the new fund would offset only one-third of rural Medicaid losses, or 5% of total projected federal Medicaid cuts.
The rural health fund is temporary, while most proposed Medicaid and ACA reductions are indefinite. Southern states like Texas, Kansas, Alabama, and Mississippi, which never fully expanded Medicaid, are expected to take the hardest hit. A 2023 KFF report found that Medicaid expansion is linked to improved financial performance among rural hospitals.
Hospitals have already begun cutting staff in response to regulatory uncertainty. UC San Diego Health recently eliminated 230 positions, citing federal policy shifts.
For more information, please visit: